Affecting millions of people worldwide, many sufferers have trouble distinguishing between psoriasis and eczema. That’s because both are autoimmune conditions that cause the skin to be itchy, dry, and red.
Not only that, but both rashes tend to appear in the same places on the body – like the hands and scalp.
In this post, we’ll discuss the features of eczema and psoriasis to help you find a treatment plan that works for your condition.
Understanding Eczema
Eczema is a chronic condition that comes in many forms. The most common types are atopic dermatitis, contact dermatitis, nummular eczema, and seborrheic dermatitis.
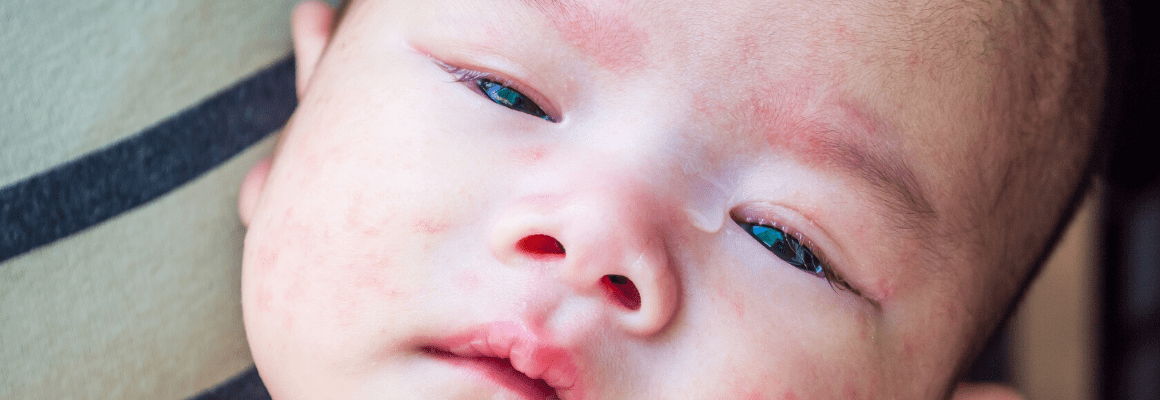
In general, eczema causes the skin to appear dry, red, and inflamed. Blisters may also develop. If intense scratching persists, the skin can even develop a rough or leathery texture. The most common places for eczema include the creases of elbows and knees, hands, and nape of the neck.
Understanding Psoriasis
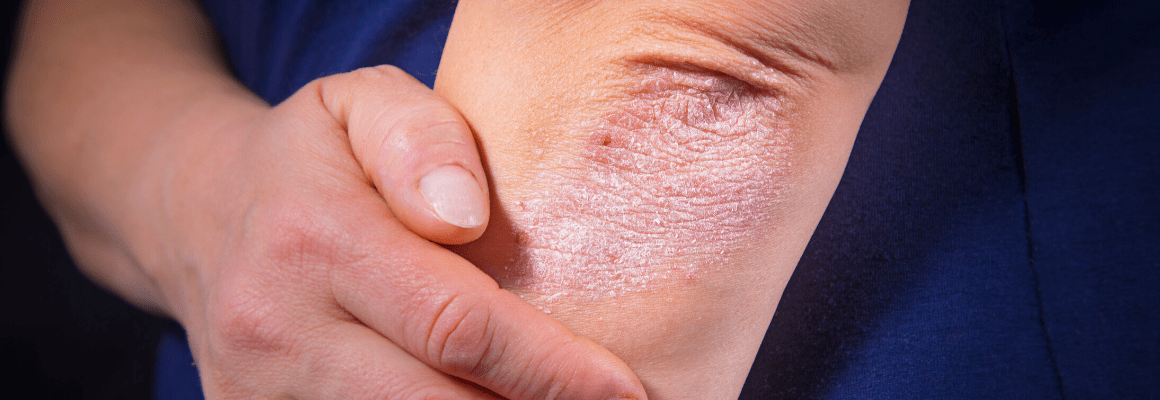
Psoriasis is also a chronic condition. It develops because of an overactive immune system that causes the skin cells to reproduce every 3-4 days. This increased production of skin cells is what causes the flaky, red patches with silvery scales to form.
While the patches can appear anywhere on the body, they typically can be found on the elbows, scalp, knees, and lower back. If left untreated or if subject to excessive scratching, the skin can creak or bleed, possibly leading to infection.
Psoriasis and Eczema Difference
Although symptoms appear similar between the two conditions, it’s important to understand their differences. With psoriasis, you may notice nail abnormalities, joint pain, and swelling or stiffness. Caused by psoriatic arthritis, stiffness in the joints is a characteristic generally not seen in eczema sufferers. The exact causes of both conditions are both unknown but they're believed to be triggered by a variety of factors and conditions.
Common triggers include stress, alcohol, extreme weather conditions, and even certain foods. Symptoms of both conditions can range from mild to severe. Neither condition is contagious or caused by poor hygiene. One of their key points of differentiation is the onset of their symptoms. Eczema is known to develop in childhood while symptoms of psoriasis typically appear when a person is between 15 and 35 years old. According to The American Academy of Dermatology, approximately 1% of children have psoriasis, while 10% of children have eczema.
Natural Treatments
While neither condition has a cure, there are ways to treat and soothe symptoms to help improve quality of life. Because of the sensitivity of skin associated with both eczema and psoriasis, gentle and natural treatments are best to avoid further aggravating the condition. Medications may differ a bit between the two conditions, but if you're looking for natural treatments, they are the same for both eczema and psoriasis.
Moisturize
Combat the itch by keeping dry skin hydrated. Our recommendation is this Organic Manuka Skin Soothing Cream. An oil-based balm, it’s great at moisturizing even the driest of skin while keeping plaque or scaling under control. Plus, it’s perfect for sensitive skin as it’s made with just six, all-natural ingredients, including Manuka honey and Manuka oil which are both high in anti-inflammatory and anti-bacterial properties.
Wear Skin-Friendly Clothing
Both conditions require soft and breathable clothing to avoid further irritating sensitive skin. Cotton and TENCEL are both excellent choices. We developed Remedywear™ specifically to treat and soothe eczema and psoriasis. Made with soft, soothing TENCEL™ and embedded with anti-inflammatory zinc, Remedywear not only reduces itching and soothes irritation, but also helps improve the quality of sleep. If scratching causes the skin to crack or bleed, zinc helps reduce the risk of infection by inhibiting the growth of bacteria. Check out our Remedywear favorites:
Dry Wrap Therapy
Dry wrap therapy provides long-term relief for flare-ups and protects against scratching. It’s easy to do: apply a natural moisturizer and cover with clothing or a hypoallergenic sleeve. For optimal effects, wear the garment overnight or for a minimum of two hours.
Change your Diet
Finally, you can also improve your skin by changing your diet. As both are inflammatory conditions, it makes sense to reduce your intake of inflammatory foods and increase your consumption of anti-inflammatory foods. Foods that cause inflammation include red meat, refined sugar, gluten, and dairy. Foods that can help reduce flare-ups include fatty fish, leafy greens, and olive oil.
References:
https://www.healthline.com/health/psoriasis-vs-eczema-pictures https://www.pennmedicine.org/updates/blogs/health-and-wellness/2019/august/psoriasis